Study in journal Cell Chemical Biology highlights need for new treatment approaches
Cleveland Clinic News Service | 216.444.0141
We’re available to shoot custom interviews & b-roll for media outlets upon request.
CCNS health and medical content is consumer-friendly, professional broadcast quality (available in HD), and available to media outlets each day.

Cleveland Clinic researchers have shown for the first time how a class of advanced prostate cancer drugs are processed in the body and how their anti-tumor activity might change depending on how they are metabolized. Their pre-clinical findings, just published in Cell Chemical Biology, may lay the foundation for improving therapies for treatment-resistant, aggressive prostate cancer.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/4f6696c0-a86d-4c4c-9fcd-b23a2df8c4b9/120074_02-22-17_549_DG_jpg)
Mohammad Alyamani, Ph.D., with lab technician Yoon-Mi Chung.
Next-generation anti-androgens are potent drugs that work by cutting off the prostate tumor’s supply of androgens (male hormones), which fuel prostate cancer. The drugs, used in patients whose cancer has become resistant to hormone deprivation therapy, have been shown to improve survival in men with metastatic disease. Unfortunately, prostate tumors eventually become resistant to these drugs, highlighting the need for new therapies.
“Despite an array of improved treatment options that have become available over the past decade, prostate cancer remains the second leading cause of cancer mortality in men in the United States. There are few therapeutic options for men whose cancer has become resistant to all therapies,” said Nima Sharifi, M.D., lead author on the study. “Our goal is to improve the use and role of these existing drugs and hopefully design new therapies that work better and longer.”
Galeterone is a steroidal anti-androgen that was recently studied in a clinical trial. Dr. Sharifi’s team in the Cleveland Clinic Lerner Research Institute’s Department of Cancer Biology has shown that when galeterone is metabolized, it is converted to the intermediate molecule D4G, which blocks androgen synthesis and reduces the amount of androgens available to cancer cells. A pitfall is that galeterone is also converted to another molecule that may stimulate the tumor.
Dr. Sharifi previously found that another steroidal anti-androgen drug, abiraterone, is metabolized in a similar manner. He went on to show in landmark studies that abiraterone’s metabolite D4A has greater anti-tumor activity than abiraterone alone and that other molecules stimulate tumor growth, suggesting that the drug should be fine-tuned to improve efficacy.
Dr. Sharifi’s new findings suggest that effective steroidal anti-androgens share common metabolic activities and that their metabolites should be closely examined for their effects on tumor survival. The findings may also guide medical decision making in the use of steroidal vs. nonsteroidal drugs for advanced prostate cancer.
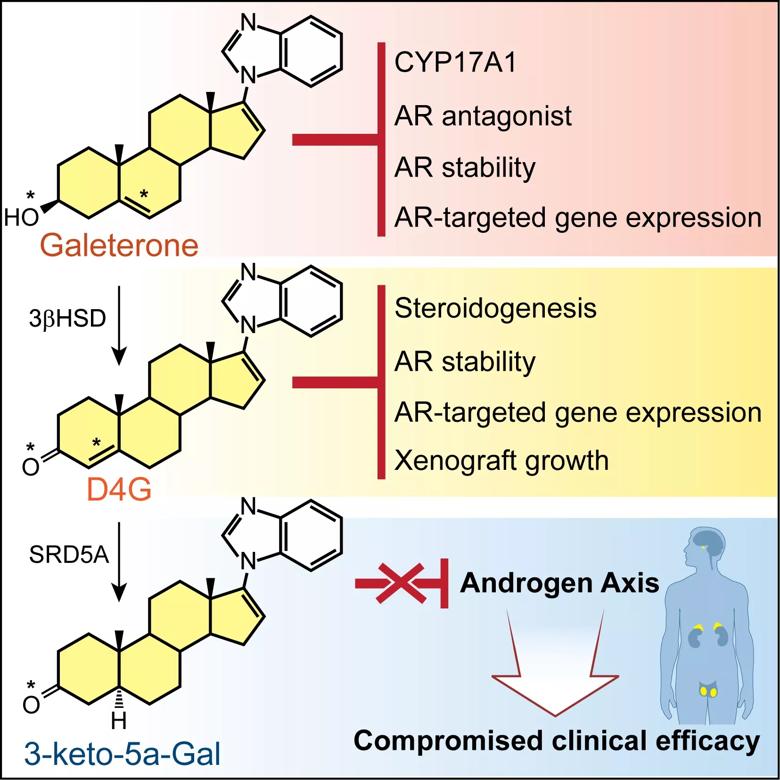
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/825b4155-c943-4c96-aaa0-b6e02d10ea8a/sharifi-GRAPHICAL_ABSTRACT_GALETERONE_SHARIFI-2_border-003_jpg)
“New agents and a clearer understanding of drug mechanisms are both urgently required to improve outcomes for treatment-resistant advanced prostate cancer,” said Dr. Sharifi. “This work provides an important foundation that hopefully will lead to better treatment strategies for this disease.”
Mohammad Alyamani, Ph.D., and Zhenfei Li, Ph.D., of Lerner Research Institute are first authors on the paper. Dr. Sharifi is also a member of the Glickman Urological & Kidney Institute and Taussig Cancer Institute of Cleveland Clinic. He holds the Kendrick Family Chair for Prostate Cancer Research at Cleveland Clinic.
This work has been supported in part by funding from a Howard Hughes Medical Institute Physician-Scientist Early Career Award, a Prostate Cancer Foundation Challenge Award, an American Cancer Society Research Scholar Award, grants from the National Cancer Institute (R01CA168899, R01CA172382, and R01CA190289), and a grant from the US Army Medical Research and Materiel Command, a Prostate Cancer Foundation Young Investigator Award.
Cleveland Clinic is a nonprofit multispecialty academic medical center that integrates clinical and hospital care with research and education. Located in Cleveland, Ohio, it was founded in 1921 by four renowned physicians with a vision of providing outstanding patient care based upon the principles of cooperation, compassion and innovation. Cleveland Clinic has pioneered many medical breakthroughs, including coronary artery bypass surgery and the first face transplant in the United States. Cleveland Clinic is consistently recognized in the U.S. and throughout the world for its expertise and care. Among Cleveland Clinic’s 82,600 employees worldwide are more than 5,786 salaried physicians and researchers, and 20,700 registered nurses and advanced practice providers, representing 140 medical specialties and subspecialties. Cleveland Clinic is a 6,728-bed health system that includes a 173-acre main campus near downtown Cleveland, 23 hospitals, 280 outpatient facilities, including locations in northeast Ohio; Florida; Las Vegas, Nevada; Toronto, Canada; Abu Dhabi, UAE; and London, England. In 2024, there were 15.7 million outpatient encounters, 333,000 hospital admissions and observations, and 320,000 surgeries and procedures throughout Cleveland Clinic’s health system. Patients came for treatment from every state and 112 countries. Visit us at clevelandclinic.org. Follow us at x.com/CleClinicNews. News and resources are available at newsroom.clevelandclinic.org.
Editor’s Note: Cleveland Clinic News Service is available to provide broadcast-quality interviews and B-roll upon request.