Research aims to identify differences in survival among heart failure patients before and after heart transplantation, as well as create tools to improve outcomes
Cleveland Clinic News Service | 216.444.0141
We’re available to shoot custom interviews & b-roll for media outlets upon request.
CCNS health and medical content is consumer-friendly, professional broadcast quality (available in HD), and available to media outlets each day.


Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/315c0716-e4c0-43c5-ad0a-694d2f6d7150/Hsich_Eileen_703878_jpg)
Eileen Hsich, M.D.
The National Institutes of Health has awarded Cleveland Clinic researcher Eileen Hsich, M.D., $2.8 million over four years to evaluate disparities in survival among heart failure patients before and after heart transplantation and to create tools that would optimize outcomes.
“We believe that to improve care for those with heart failure awaiting transplant, we must better understand how differences among patients affect the timing of transplants and survival. With this knowledge, we can create innovative models that can help physicians decide the best time for individual patients to be transplanted,” said Dr. Hsich. “The findings from these research projects will hopefully lay the groundwork for a dynamic and improved way to allocate hearts in the future.”
Heart failure affects 6.5 million Americans, and many need advanced care such as circulatory support devices or transplant. However, due to a shortage of organs, numerous people die each year waiting for a heart. Currently, about 4,000 patients are waiting for heart transplants, and in 2017, surgeons performed about 3,200 heart transplants.
The grant will be used for three research projects:
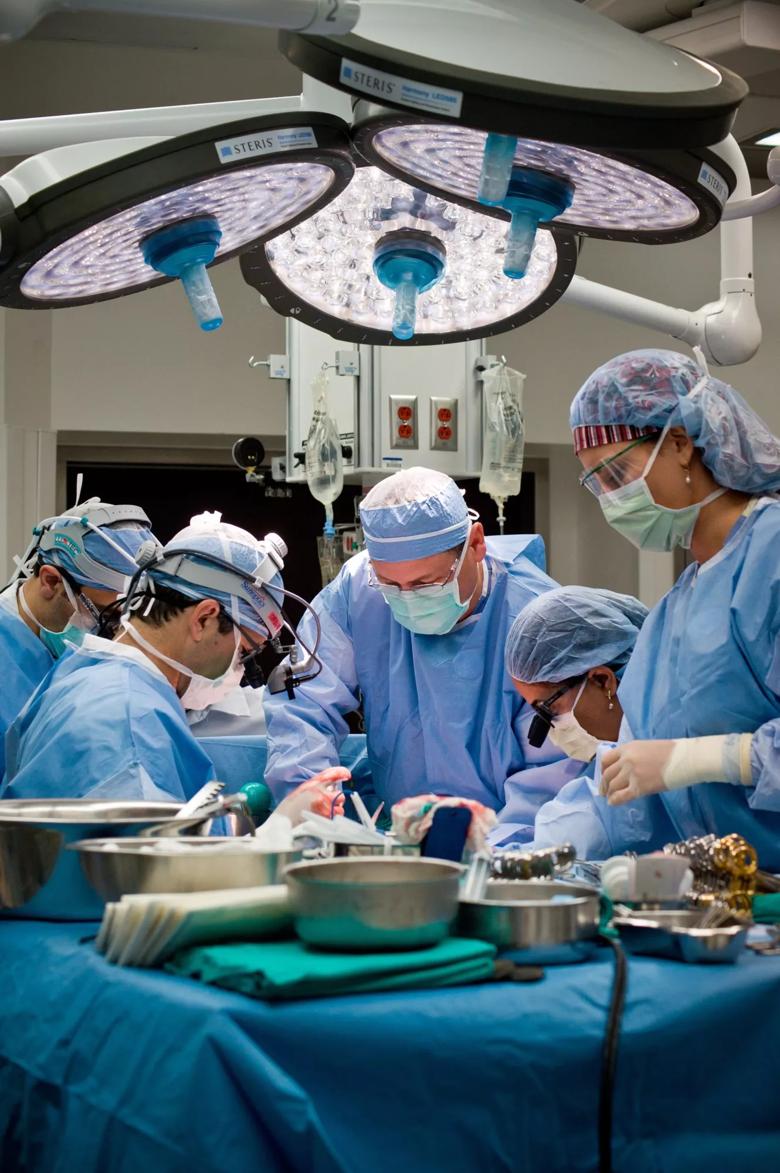
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/334e4e91-82ec-4a5e-ba7a-52d9edd71a00/heart-transplant_full-7002913-scaled_jpg)
This work with will build upon other studies by Dr. Hsich investigating disparities in heart transplant patients. Her previous research has identified differences in heart transplant waiting list survival based on type of heart disease. Other research that she has led confirmed that despite shorter times on the list, women have higher mortality compared to men waiting urgently for heart transplants.
Cleveland Clinic is a nonprofit multispecialty academic medical center that integrates clinical and hospital care with research and education. Located in Cleveland, Ohio, it was founded in 1921 by four renowned physicians with a vision of providing outstanding patient care based upon the principles of cooperation, compassion and innovation. Cleveland Clinic has pioneered many medical breakthroughs, including coronary artery bypass surgery and the first face transplant in the United States. Cleveland Clinic is consistently recognized in the U.S. and throughout the world for its expertise and care. Among Cleveland Clinic’s 82,600 employees worldwide are more than 5,786 salaried physicians and researchers, and 20,700 registered nurses and advanced practice providers, representing 140 medical specialties and subspecialties. Cleveland Clinic is a 6,728-bed health system that includes a 173-acre main campus near downtown Cleveland, 23 hospitals, 280 outpatient facilities, including locations in northeast Ohio; Florida; Las Vegas, Nevada; Toronto, Canada; Abu Dhabi, UAE; and London, England. In 2024, there were 15.7 million outpatient encounters, 333,000 hospital admissions and observations, and 320,000 surgeries and procedures throughout Cleveland Clinic’s health system. Patients came for treatment from every state and 112 countries. Visit us at clevelandclinic.org. Follow us at x.com/CleClinicNews. News and resources are available at newsroom.clevelandclinic.org.
Editor’s Note: Cleveland Clinic News Service is available to provide broadcast-quality interviews and B-roll upon request.