HoloLens technology helping shape face transplant surgery and treatment for cancer and aortic aneurysms
Cleveland Clinic News Service | 216.444.0141
We’re available to shoot custom interviews & b-roll for media outlets upon request.
CCNS health and medical content is consumer-friendly, professional broadcast quality (available in HD), and available to media outlets each day.
images: 0
video: 0
audio: 0
text: 0
Augmented reality is the use of computer technology to visually expand a user’s environment. It’s transforming countless industries, from gaming to retail, and, increasingly, the practice of medicine, too.
A form of augmented reality is being adapted by Cleveland Clinic research scientists and physicians for use in a wide array of clinical applications. Doctors are using a fully self-contained holographic computer –the Microsoft HoloLens augmented reality device –to enhance the treatment of liver cancer, aortic aneurysms, ovarian cancer and even face transplant surgery.
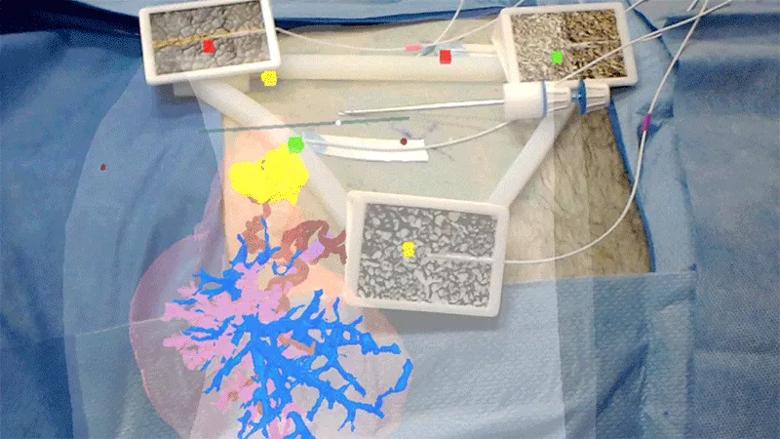
Most recently, HoloLens has been incorporated into liver cancer treatment. A Cleveland Clinic research team recently launched a first-of-its-kind clinical trial evaluating the technology for improving the accuracy and effectiveness of a minimally-invasive thermal therapy (microwave ablation) to destroy liver tumors.
“This is the first time in the world, to our knowledge, extended reality surgical navigation has been evaluated in a liver tumor ablation procedure,” said Karl West, director of medical device solutions at Cleveland Clinic’s Lerner Research Institute and one of the inventors of the technology. “HoloLens provides an entirely different way to visualize the tumor’s location. It is a paradigm shift and may have potential applications for a variety of other procedures and diseases.”
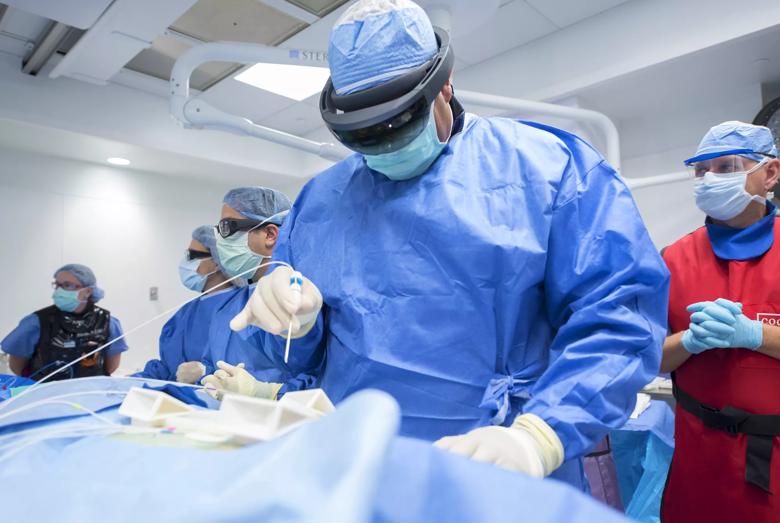
The study is comparing 2D standard of care images, displayed on a conventional flat panel screen, with 3D holographic images, which layer virtual projections on top of the user’s real-world view. This enables the medical team to see the patient’s specific anatomy in 3D. This 3D holographic image is projected onto the patient, giving the doctor “X-ray vision” to better visualize the path to the tumor.
Using the holographic image, the radiologist guides a biopsy needle into the tumor with enhanced precision. The team then delivers microwave energy through the needle, to heat and destroy the abnormal tumor tissue. Throughout the procedure, the physician uses head–mounted glasses to see the patient’s internal anatomical structures and verify tumor location with the technology’s mini-global positioning (GPS)-like system.
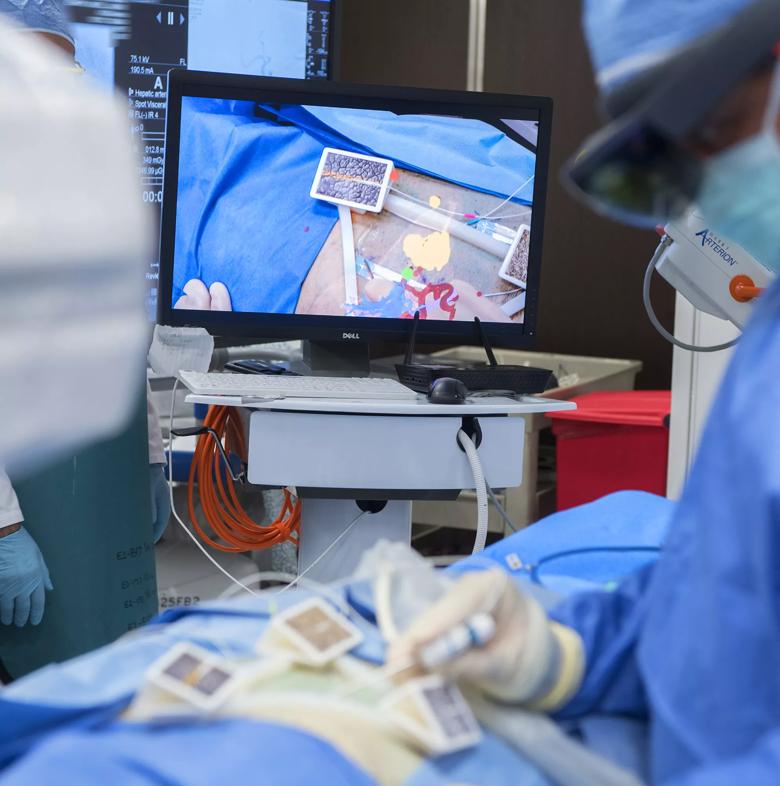
“We are assessing if this augmented reality system can overcome the limitations of displaying images such as ultrasound, fluoroscopy and CT on 2D flat screens,” said Charles Martin III, M.D., director of interventional oncology, in the Department of Radiology, at Cleveland Clinic. “The transformative technology allows a physician to see the patient’s anatomy in a completely unique way. I feel it can assist in enhancing minimally invasive therapies for patients. It provides an unprecedented ability to better visualize the patient’s anatomical structures and map out the most precise path to the tumor in real time.”
Cleveland Clinic’s surgical team was the first-ever to use HoloLens technology during an extremely complex total face transplant surgery, on the youngest patient in the United States to undergo the procedure.
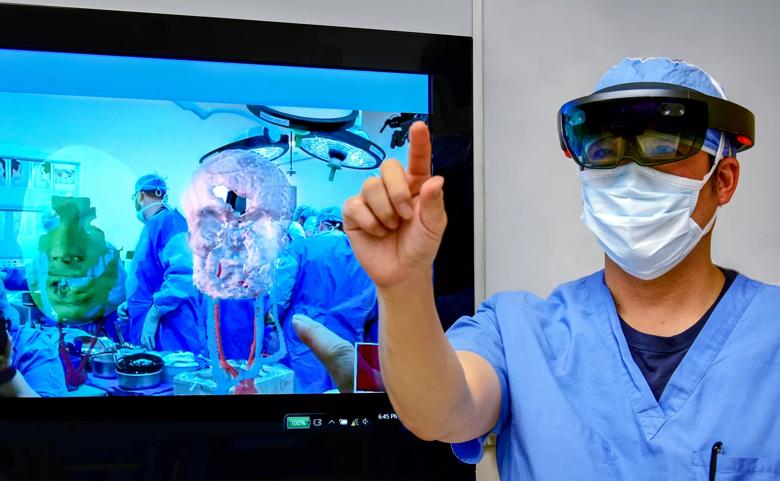
RELATED: How Augmented Reality Shaped Cleveland Clinic’s Total Face Transplant
In 2017, the surgical team used the HoloLens headset to overlay a 3D holographic representation of the donor’s anatomy onto the recipient’s face to assess alignment and refine their surgical plans.
In addition to liver tumor ablation, Cleveland Clinic is incorporating the virtual reality technology for aortic aneurysm treatment. Researchers are studying the ability of HoloLens to enhance accuracy in improving stent placement. Cleveland Clinic and Centerline Biomedical, a Cleveland Clinic spin-off company, were awarded a National Institutes of Health (NIH) grant to test a “holographic GPS system for the OR” that enables 3D-visualization during minimally invasive procedures.
RELATED: “GPS System for the Operating Room” to Be Tested in Patient-Specific Models
The technique includes the use of Centerline’s novel Intra-operative Positioning System (IOPS) coupled with HoloLens to visualize the procedure in true 3D (as opposed to traditional 2D X-ray). The researchers are using IOPS to control and more precisely place the stent graft within an aortic aneurysm, or other vascular lesion, thereby reducing radiation exposure and decreasing procedure time.
Cleveland Clinic is a nonprofit multispecialty academic medical center that integrates clinical and hospital care with research and education. Located in Cleveland, Ohio, it was founded in 1921 by four renowned physicians with a vision of providing outstanding patient care based upon the principles of cooperation, compassion and innovation. Cleveland Clinic has pioneered many medical breakthroughs, including coronary artery bypass surgery and the first face transplant in the United States. Cleveland Clinic is consistently recognized in the U.S. and throughout the world for its expertise and care. Among Cleveland Clinic’s 81,000 employees worldwide are more than 5,743 salaried physicians and researchers, and 20,160 registered nurses and advanced practice providers, representing 140 medical specialties and subspecialties. Cleveland Clinic is a 6,690-bed health system that includes a 173-acre main campus near downtown Cleveland, 23 hospitals, 276 outpatient facilities, including locations in northeast Ohio; Florida; Las Vegas, Nevada; Toronto, Canada; Abu Dhabi, UAE; and London, England. In 2023, there were 13.7 million outpatient encounters, 323,000 hospital admissions and observations, and 301,000 surgeries and procedures throughout Cleveland Clinic’s health system. Patients came for treatment from every state and 132 countries. Visit us at clevelandclinic.org. Follow us at twitter.com/CleClinicNews. News and resources available at newsroom.clevelandclinic.org.
Editor’s Note: Cleveland Clinic News Service is available to provide broadcast-quality interviews and B-roll upon request.