Just one previously reported case resulted in continued pregnancy, successful delivery
Content is property of Cleveland Clinic and for news media use only.

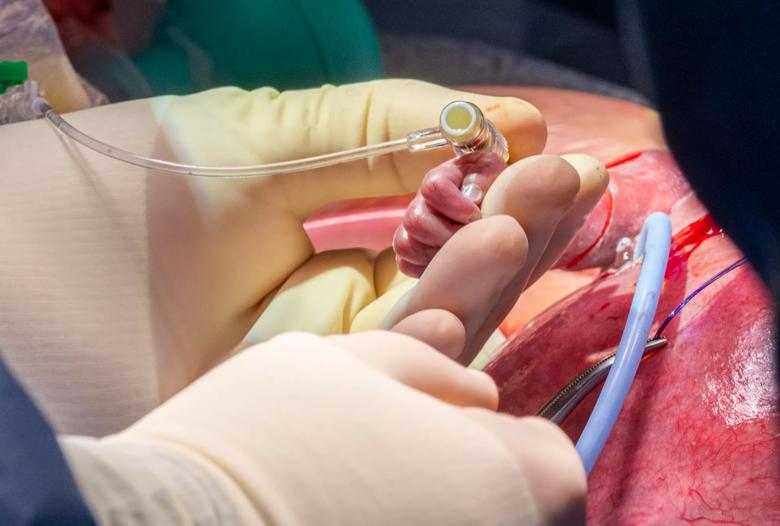
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/1a708036-fee5-41f5-bf52-43aa9952812c/CCC_2149658_05-07-21_396_MLC-crop-scaled_jpg)
Hani Najm, M.D., who led the heart surgery team, inserts an IV line in the fetus’s right arm to deliver fluids and medications as needed. (Courtesy: Cleveland Clinic)
A multidisciplinary team of Cleveland Clinic and Cleveland Clinic Children’s doctors and nurses performed a rare and complex lifesaving fetal surgery to remove a tumor attached to the heart of a 26-week-old fetus.
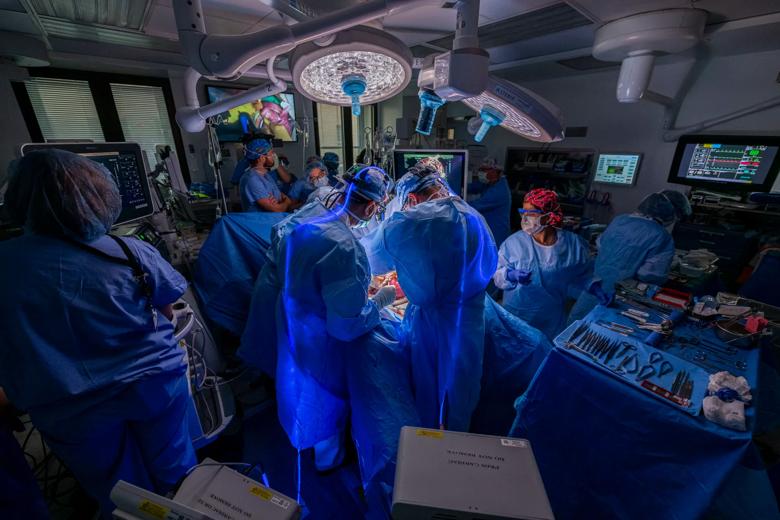
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/8699a620-9805-4f37-8884-c3a281d78dd6/CCC_2149658_05-07-21_387_MLC-scaled_jpg)
The surgery included pediatric and congenital heart surgeons, a pediatric cardiologist, obstetric and pediatric anesthesiologists, and a maternal-fetal medicine specialist. (Courtesy: Cleveland Clinic)
Few studies about the rare condition – an intrapericardial teratoma with fetal hydrops (i.e., fluid accumulation) evolving to fetal heart failure – have been reported in medical journals. “Only one previous incidence of continued pregnancy and delivery after fetal intrapericardial teratoma resection is documented in the world’s medical literature,” said Darrell Cass, M.D., director of Cleveland Clinic’s Fetal Surgery and Fetal Care Center. “As far as we know, Cleveland Clinic is the second academic medical center in the world to have performed this fetal surgery successfully with continued pregnancy and delivery.”
During the procedure in May, surgeons successfully removed the malignant tumor, which had been compressing the left side of the fetus’ heart and impairing circulation, leading to fluid accumulation around the heart and other organs of the fetus.
Following the operation, the mother and fetus recovered well with no complications and no sign of tumor recurrence during prenatal check-ups. On July 13, at 36 weeks and two days, a baby boy was delivered near full term by Cesarean section. Both mother and baby are doing well.
“I am very proud of our talented congenital heart surgery and fetal surgery teams that integrated seamlessly to successfully perform a complex lifesaving fetal surgery,” said Dr. Cass. “This tumor was growing rapidly in the exact wrong spot. It was compressing the heart of the fetus, causing fluid accumulation, and we started seeing signs that the cardiac function was deteriorating. We needed to act quickly and decisively to rescue the fetus.”
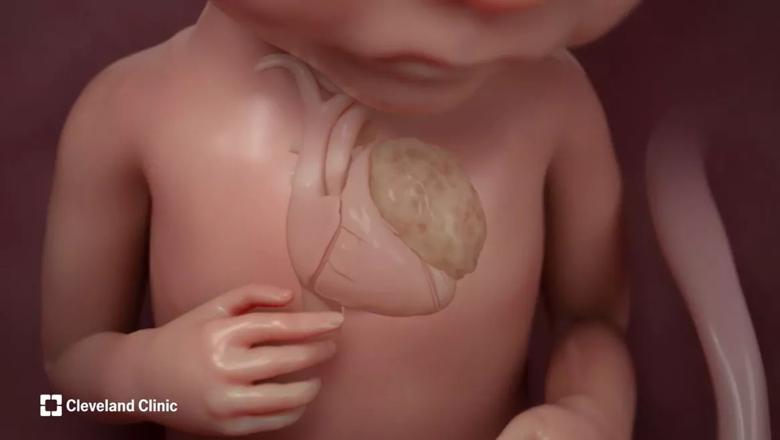
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/8038f362-91fc-449e-a362-d93cede174b2/fetal-Capture_jpg)
Click on the image to view or download an animation of the fetal intrapericardial teratoma resection.
To perform this fetal surgery, Dr. Cass led a team that included pediatric and congenital heart surgeons Hani Najm, M.D., and Alistair Phillips, M.D.; pediatric cardiologist Francine Erenberg, M.D.; obstetric and pediatric anesthesiologists McCallum Hoyt, M.D., Tara Hata, M.D., Yael Dahan, M.D.; and maternal-fetal medicine specialist, Amanda Kalan, M.D., who provided the mother’s care, including delivery of the newborn baby boy 10 weeks after the fetal surgery.
Once the mother was anesthetized with an approach to provide the safest environment for the fetal heart surgery to be successful, a Cesarean section-like incision was made to expose the mother’s uterus. Ultrasound was used to carefully locate the placenta and fetus, and best location for entry. The uterus was then opened about 12 cm, and the arms of the fetus were brought out to expose the chest.
Dr. Najm, who led the heart surgery team, inserted an IV line in a blood vessel of the fetus’s right arm to deliver fluids and medications as needed. Then, he carefully opened the chest and pericardium, which is the membrane enclosing the heart, and removed the tumor from the beating fetal heart. “As soon as the tumor was removed, the compression of the left atrium disappeared, and there was a nice blood flow that was almost back to normal,” said Dr. Najm.
Following the completion of the fetal heart surgery, the chest of the fetus was closed and the fetus was positioned back in the uterus. The uterus was then closed, followed by closure of the mother’s abdomen. The surgery lasted 3 ½ hours.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/fcb76057-80e7-4a2d-9950-428edc94cd9c/CCC_2331308_08-13-21_0094_AMO-scaled_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/0c764f71-dfa6-4728-9cfa-21034409767f/CCC_2409013__10-17-21_028_AMO-scaled_jpg)
Rylan Harrison Drinnon was born on July 13 to Sam and Dave Drinnon.
Both mother and fetus recovered well following the surgery. The fetus’s cardiac function immediately improved, and the fetus stayed in the womb for the remainder of the pregnancy. Ten weeks later, the baby was born.
“Such an innovative fetal surgery provides hope to other families who may receive a similar devastating diagnosis,” said Dr. Najm, chair of Pediatric and Congenital Heart Surgery at Cleveland Clinic Children’s. “Clinical teams from Cleveland Clinic and Cleveland Clinic Children’s are consistently collaborating and remain dedicated to innovation and teamwork to ensure our patients of all ages can feel safe when entrusting their care to us.”
Moving forward, the infant’s healthcare team will monitor his heart health and check that there are no signs of tumor recurrence. In the future, the child will likely need surgery to reposition together his sternum that did not properly heal in utero.
“In this case, time was of the essence,” said Dr. Cass. “Shortly after the patient arrived at Cleveland Clinic, imaging tests showed that the tumor kept growing and the fetus’s heart function was deteriorating. It is important to acknowledge the whole care team. This family’s maternal fetal medicine specialist accurately diagnosed the condition and reached out to us because of our expertise in fetal care and treatment.”
Cleveland Clinic is a nonprofit multispecialty academic medical center that integrates clinical and hospital care with research and education. Founded in 1921 by four renowned physicians with a vision of providing outstanding patient care based upon the principles of cooperation, compassion and innovation, Cleveland Clinic has pioneered many medical breakthroughs, including coronary artery bypass surgery and the first face transplant in the United States. Cleveland Clinic is consistently recognized in the U.S. and throughout the world for its expertise and care. Among Cleveland Clinic’s 83,000 employees worldwide are more than 6,600 salaried physicians and researchers, and 21,900 registered nurses and advanced practice providers, representing 140 medical specialties and subspecialties. Cleveland Clinic is a 6,725-bed health system that includes a 173-acre main campus near downtown Cleveland, 23 hospitals, 300 outpatient facilities, including locations in northeast Ohio; Florida; Las Vegas, Nevada; Toronto, Canada; Abu Dhabi, UAE; and London, England. In 2025, there were 15.9 million outpatient encounters, 343,000 hospital admissions and observations, and 336,000 surgeries and procedures throughout Cleveland Clinic’s health system. Visit us at clevelandclinic.org. Follow us at x.com/CleClinicNews. News and resources are available at newsroom.clevelandclinic.org.
Editor’s Note: Cleveland Clinic News Service is available to provide broadcast-quality interviews and B-roll upon request.