Cleveland Clinic News Service | 216.444.0141
We’re available to shoot custom interviews & b-roll for media outlets upon request.
CCNS health and medical content is consumer-friendly, professional broadcast quality (available in HD), and available to media outlets each day.

While nursing Scarlett, her 5-month-old daughter, Heather Kokinda noticed a lump in one of her breasts. She decided to have it checked, but wasn’t really concerned.
“I thought it was a clogged milk duct,” she said. “When you’re 29, you don’t think it’s breast cancer.”
But it was. X-rays and a biopsy revealed the shocking news that the Seville, Ohio resident had Stage 1 breast cancer. “I went from feeling my life was perfect as a new mom, to the world crashing down around me,” Heather recalled.
RELATED: Cleveland Clinic Research Links Breast Cancer to Bacterial Imbalance
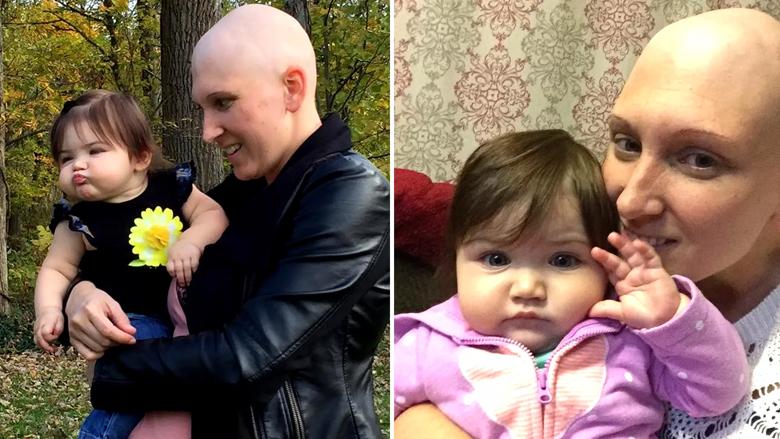
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/0fb28e00-f1e5-4211-913c-cb6494c11376/heather-cancer-baby-tease-10232017_jpg)
Heather Kokinda, a Cleveland Clinic patient, with her daughter Scarlett.
By the time she began treatment with breast cancer oncologist Dr. Halle Moore at Cleveland Clinic Cancer Center, just two weeks later, the fast-growing disease had progressed to Stage 2. Because chemotherapy is the standard treatment for her type of breast cancer, and a common side-effect is ovarian failure, Heather knew the likelihood of having another child was slim.
RELATED: Preparing For The Most Unexpected Body Change After Breast Cancer
“I came to terms with that,” Heather explained. “I had my daughter, and that was good enough for me.”
And yet, less than two years later, a healthy Heather is now the mother of two daughters. Scarlett’s sister, Josslyn, was born in July 2017 – thanks in part to a pioneering treatment Dr. Moore has helped spearhead that can protect the ovaries from the effects of chemotherapy.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/40322fcc-3833-418d-bfea-e27449730582/heather-family-fertility2-10232017_jpg)
Heather Kokinda, a Cleveland Clinic patient, with her daughter Scarlett.
Heather agreed to receive a drug called goserelin, a synthetic version of a naturally-occurring hormone, by monthly injections into the abdomen during chemotherapy. It temporarily suppresses the function of the ovaries, serving to protect them from premature menopause and infertility that can be caused by chemotherapy.
RELATED: Cleveland Clinic Research: How Often are Breast Cancer Patients Referred to Fertility Experts?
“Some young women are unwilling to take chemotherapy if their fertility will be impaired,” noted Dr. Moore, the lead author of a study on the effectiveness of goserelin that was published in the New England Journal of Medicine. “It can be quite dangerous to choose not to move forward, because chemo could vastly improve a patient’s likelihood of long-term survival.”
While women of child-bearing age also have the option of more traditional assistive reproduction techniques, such as storing embryos and eggs, these invasive and often expensive procedures can be an added burden while enduring cancer treatment. As Dr. Moore explained, the goserelin injections “provide women with another fertility option.”
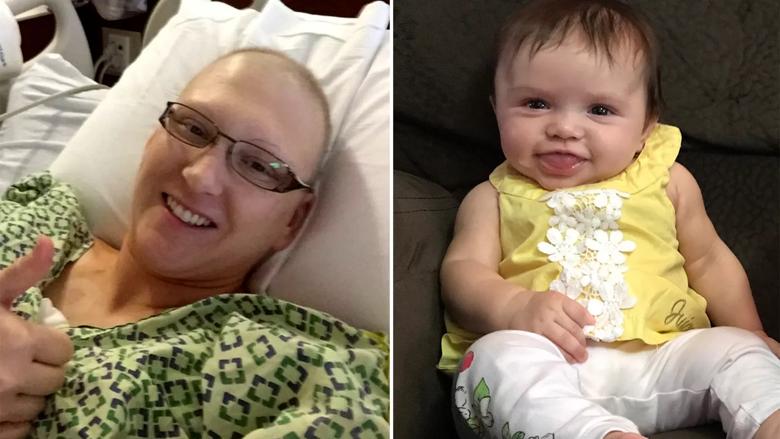
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/436ba6b2-3c6f-4dea-a3cf-b8169caeb4f6/heather-daughter-split-10242017_jpg)
Heather Kokinda, a Cleveland Clinic patient, with her daughter Scarlett.
The study Dr. Moore led – the Prevention of Early Menopause Study (POEMS) – found patients who received goserelin during chemotherapy experienced just an 8 percent ovarian failure rate, about one-third the rate for the control group not receiving the treatment. Further, twice as many women gave birth after having goserelin treatments than those in the control group.
Video content: This video is available to watch online.
View video online (https://www.youtube.com/embed/-xOrQVrAHZY?feature=oembed&wmode=transparent)
While Heather describes the four monthly injections as relatively painless, she did experience the typical effects associated with menopause while her ovaries were temporarily shut down. “Oh, I had hot flashes and everything,” Heather noted. “But it was worth it.”
While Dr. Moore recommends most women treated with chemotherapy wait at least two years before trying to conceive, to ensure they make it through the highest-risk period for an aggressive recurrence, Heather was pregnant about a year after completing chemotherapy, a double mastectomy and reconstructive surgeries.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/7a845ead-6b9d-497a-bb7b-689bcbd3885c/heather-family-fertility-10232017_jpg)
Heather Kokinda, a Cleveland Clinic patient, with her daughter Scarlett.
Now cancer-free, she and husband Jeremy are happily parenting two very active daughters. “The option to protect my fertility gave me the possibility to have another child,” Heather said, “without having to go through great lengths to do so. It’s pretty amazing.
Cleveland Clinic is a nonprofit multispecialty academic medical center that integrates clinical and hospital care with research and education. Founded in 1921 by four renowned physicians with a vision of providing outstanding patient care based upon the principles of cooperation, compassion and innovation, Cleveland Clinic has pioneered many medical breakthroughs, including coronary artery bypass surgery and the first face transplant in the United States. Cleveland Clinic is consistently recognized in the U.S. and throughout the world for its expertise and care. Among Cleveland Clinic’s 83,000 employees worldwide are more than 6,600 salaried physicians and researchers, and 21,900 registered nurses and advanced practice providers, representing 140 medical specialties and subspecialties. Cleveland Clinic is a 6,725-bed health system that includes a 173-acre main campus near downtown Cleveland, 23 hospitals, 300 outpatient facilities, including locations in northeast Ohio; Florida; Las Vegas, Nevada; Toronto, Canada; Abu Dhabi, UAE; and London, England. In 2025, there were 15.9 million outpatient encounters, 343,000 hospital admissions and observations, and 336,000 surgeries and procedures throughout Cleveland Clinic’s health system. Visit us at clevelandclinic.org. Follow us at x.com/CleClinicNews. News and resources are available at newsroom.clevelandclinic.org.
Editor’s Note: Cleveland Clinic News Service is available to provide broadcast-quality interviews and B-roll upon request.